Improve your health
Improve your health
Improve your health
22 de enero de 2026
Wearables in CKD Monitoring


Wearables are changing how chronic kidney disease (CKD) is monitored and managed. These devices offer non-invasive, real-time tracking of key biomarkers like creatinine, urea, and potassium, enabling earlier detection of complications such as arrhythmias and hyperkalemia. For the 37 million Americans living with CKD, this technology reduces reliance on blood tests and clinic visits, providing a more convenient and continuous way to monitor health.
Key Takeaways:
CKD affects 15% of U.S. adults, with late diagnosis often leading to irreversible damage.
Traditional tests are expensive, time-consuming, and provide only a single snapshot of kidney health.
Wearables track biomarkers through sweat and interstitial fluid, offering continuous insights into kidney function.
Devices like the Lepu ER1 and Withings Scanwatch detect heart issues and other complications with high accuracy.
Integration with digital platforms allows remote monitoring, enabling healthcare providers to intervene earlier.
Wearables are reshaping CKD care by making monitoring more accessible, precise, and patient-friendly.
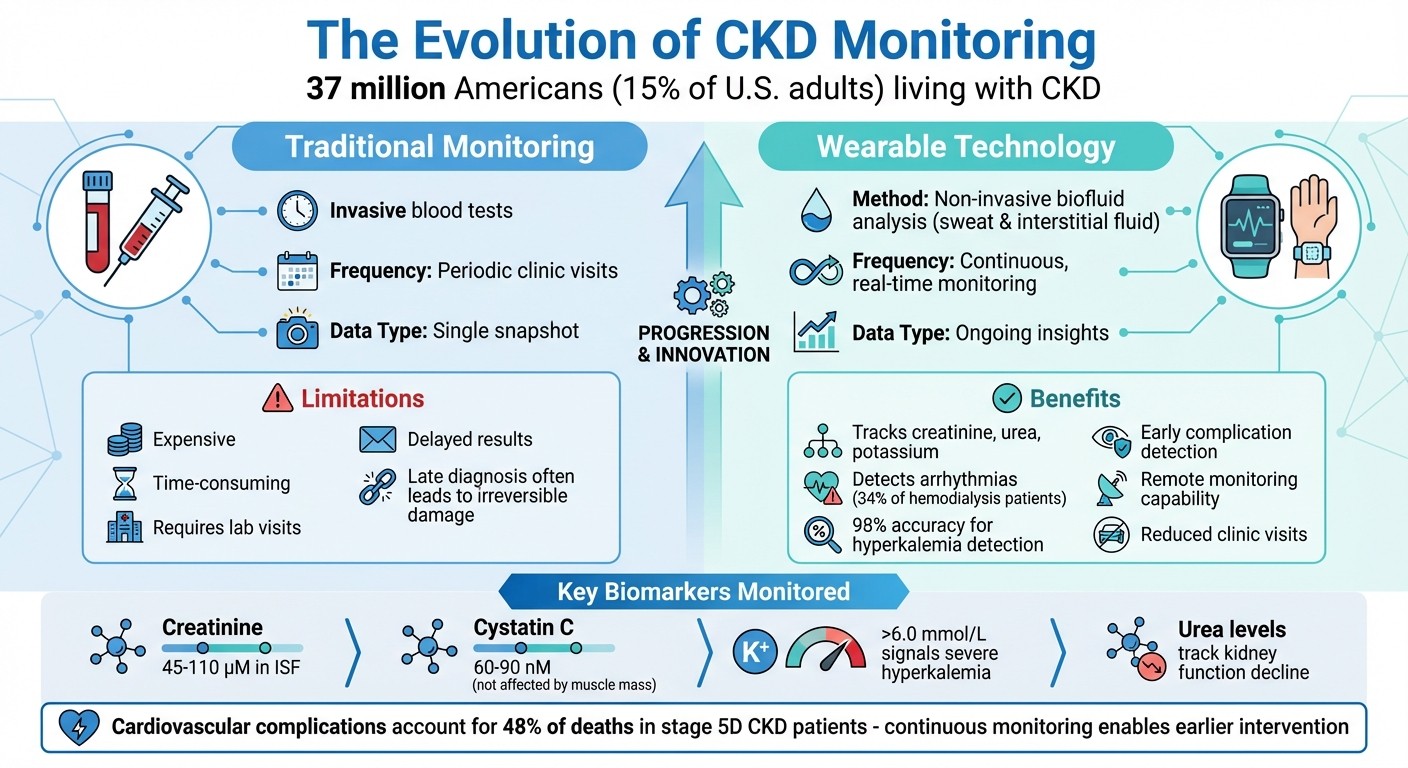
Traditional CKD Monitoring vs Wearable Technology: Key Differences and Benefits
Wearable Sensor for kidney disease
How Wearable Technologies Monitor CKD
Wearable devices are transforming kidney health monitoring by offering a non-invasive way to track key biomarkers in real time. Unlike traditional blood tests that require trips to the lab and waiting for results, these devices analyze biofluids like sweat and interstitial fluid (ISF) on the spot. This real-time monitoring makes it possible to detect changes in kidney function earlier and track biomarkers more precisely over time.
Key Biomarkers for CKD Monitoring
Wearables focus on critical biomarkers like creatinine, urea, and cystatin C to estimate eGFR, the standard measurement for kidney function. For example, creatinine - one of the most important indicators of kidney health - can be measured in ISF at levels of 45–110 μM, which closely match those found in blood. This makes ISF a practical alternative to traditional blood tests [1]. Urea levels, which increase as kidney function declines, are another key marker for managing chronic kidney disease.
Cystatin C is gaining attention as a reliable biomarker because its levels are not influenced by muscle mass. Its typical blood concentration ranges from 60–90 nM, but detecting it requires highly sensitive technology [1]. Wearables also monitor electrolytes like potassium, sodium, and calcium. For instance, potassium levels above 6.0 mmol/L signal severe hyperkalemia [3], offering insights into kidney health and overall fluid balance. These biomarkers are captured using advanced, non-invasive sensing techniques.
Non-Invasive Sensing Technologies
Modern wearable devices use cutting-edge, non-invasive methods to measure biomarkers. For instance, sweat analysis is a common approach that employs iontophoresis - a mild chemical stimulation (often with pilocarpine) - to induce sweat production even when the body is at rest [1][7]. The sweat is then analyzed using electrochemical sensors, which rely on enzymatic reactions like creatinine deiminase to break down creatinine for detection.
Another method is interstitial fluid sensing, where devices use microneedle patches or reverse iontophoresis (a small electrical current that extracts molecules) to access ISF [1][9]. This method is particularly effective for tracking larger molecules, such as cystatin C, which are less detectable in sweat.
Advances in sensor technology are improving the accuracy of these measurements. Molecularly Imprinted Polymers (MIPs), for example, act as synthetic receptors that are more stable than natural antibodies [1][9]. Similarly, Organic Electrochemical Transistors (OECTs) amplify weak signals, making it easier to detect even trace amounts of biomarkers. Some devices also incorporate colorimetric methods, where chemical reactions cause color changes that can be analyzed using smartphone cameras [1][7]. To ensure reliable results, advanced wearable patches include features like pH and sweat rate sensors to adjust readings and minimize interference.
Wearables for Tracking CKD-Related Health Metrics
Wearable devices are transforming how we monitor and manage chronic kidney disease (CKD). These gadgets continuously track vital signs that are critical for CKD care, especially since cardiovascular complications account for 48% of deaths among stage 5D CKD patients. For those dependent on dialysis, the mortality rate is a staggering 10 to 20 times higher than in the general population [4]. The constant stream of data from wearables supports precise interventions, improving both heart health and overall CKD management.
Monitoring Vital Signs and Related Conditions
Wearables are particularly effective in tracking the vital signs that help manage cardiovascular complications linked to CKD. For example, the BPM Connect provides automated blood pressure readings with a minimal margin of error - just 0.6 ± 5.3 mmHg for systolic measurements. Heart rate variability (HRV) is another critical metric. A study involving 458 patients, known as the CRIC study, demonstrated that HRV strongly predicts cardiovascular risk. It found that patients with high proteinuria had an SDNN (a key HRV metric) that was 5.73 ms lower. Those with an SDNN below 50 ms faced a 51.4% mortality risk, compared to just 5.5% for those with an SDNN above 100 ms [4][2].
Fluid management, another cornerstone of CKD care, also benefits from wearable technology. Bioimpedance sensors, like the Re:Balans used in a Norwegian study, track extracellular resistance (RE) changes during dialysis. Among 31 end-stage renal disease patients, RE increased by an average of 7.5 ± 4.3 Ω, correlating strongly (r = 0.82) with the volume of fluid removed [8]. Meanwhile, the Withings Scanwatch offers a 3% RMSE for SpO2 readings, aiding in early detection of issues like volume overload and pulmonary edema [4].
Advanced algorithms applied to wearable ECG data can even detect hyperkalemia with an accuracy of around 98% [3]. This is a game-changer, as serum potassium levels above 6.0 mmol/L are linked to significantly higher risks of complications and death. Noninvasive monitoring through wearables helps prevent such emergencies.
Stress and Sleep Tracking for CKD Patients
Wearables go beyond cardiovascular metrics, offering insights into stress and sleep - both of which are crucial for CKD care. Sleep disorders are a common issue, with 69% of maintenance hemodialysis patients experiencing insomnia, 24% dealing with obstructive sleep apnea, and 18% suffering from restless leg syndrome [4]. These issues are even more pronounced in stage 5 CKD patients and are associated with poorer quality of life and worse health outcomes.
The Withings Sleep Analyzer uses pressure sensors to track sleep stages, heart rate, and breathing patterns. It has shown 88% sensitivity and 88.6% specificity in detecting moderate-to-severe sleep apnea (AHI ≥ 15) [4].
HRV metrics also shed light on the autonomic nervous system. CKD patients with diabetes often show disrupted circadian rhythms [2][10]. Wearables can monitor nocturnal blood pressure and heart rate dipping, which, when absent, is linked to higher cardiovascular risks and mortality [2]. Additionally, advanced sensors like Organic Electrochemical Transistors (OECTs) can detect cortisol levels in sweat at nanomolar concentrations, offering insights into stress levels [1].
Platforms like Healify integrate data from wearables - covering HRV, sleep patterns, and stress markers - into actionable health plans. Healify’s AI health coach, Anna, provides personalized recommendations to help patients manage CKD and maintain cardiovascular health, creating a more holistic approach to care.
Connecting Wearable Data with Digital Health Platforms
When wearable devices sync with digital health platforms, they turn raw data into meaningful insights that can drive early medical intervention. For patients with chronic kidney disease (CKD), this integration allows healthcare providers to monitor key health trends remotely and step in before complications escalate.
Remote Monitoring and Clinical Decision Support
Wearables send data through Bluetooth, WiFi, or cellular networks to secure cloud platforms. Healthcare providers can then access this data using web dashboards that display trends, alerts, and clinical notes, offering a clear view of patient health [4][11]. This kind of connectivity is crucial - studies show that emergency visits spike tenfold in the 30 days leading up to dialysis [11].
A practical example of this approach is the VIEWER trial, conducted from November 2017 to July 2019 at Seven Oaks General Hospital in Winnipeg, Manitoba. Dr. Claudio Rigatto and his team equipped 26 advanced CKD patients (eGFR <15) with iPad minis and Bluetooth-enabled devices to monitor blood pressure, weight, and oxygen saturation. The system effectively tracked uremic symptoms and vital signs, but adherence dropped from 77.17% initially to 36% over three months. The decline was largely due to connectivity issues with Bluetooth devices and the perceived inconvenience of use [11].
The Withings RPM Solution provides another real-world application. Devices like the ScanWatch sync with a centralized cloud system where data is processed on HDS servers. Patients can view their metrics through the Health Mate app, while healthcare providers rely on a web-based interface for clinical decisions. Bernard Canaud from Fresenius Medical Care's Global Medical Office highlighted the benefits of this technology:
"technological advances had led to the development of new home-used, self-operated, connected medical devices, which offer convenient and new tools for monitoring patients in a fully automated and ambulatory mode" [4].
This seamless data integration creates a foundation for artificial intelligence (AI) systems to refine these insights and enhance patient care.
AI-Powered Analysis for CKD Management
Once wearable data is securely transmitted and aggregated, AI models step in to turn these metrics into actionable clinical insights. For instance, Convolutional Neural Networks (CNNs) can process raw sensor data - like ECG waveforms - to detect specific health issues without manual input [3]. Notably, 80.8% of arrhythmias identified by wearable ECG monitors in hemodialysis patients were asymptomatic, highlighting the importance of continuous AI-driven monitoring [6].
Between March 2022 and October 2023, researchers at the West China Biomedical Big Data Center of Sichuan University developed an advanced monitoring system for over 500 hemodialysis patients. Using a wearable chest strap ECG paired with a 1D-CNN model, the system achieved 98.25% accuracy and 98.63% sensitivity in identifying serum potassium levels above 6.0 mmol/L. This high level of precision enables timely interventions to prevent life-threatening hyperkalemia [3].
Healify takes this integration a step further by combining wearable data with personalized AI-driven insights. The app’s AI health coach, Anna, analyzes metrics like heart rate variability, sleep patterns, and stress levels alongside other biometrics and lifestyle factors. This comprehensive analysis provides 24/7 tailored recommendations, helping CKD patients manage their condition with clear, actionable plans that simplify complex health data.
The Future of Wearables in CKD Monitoring
New Developments in Wearable Biosensors
Advancements in wearable technology are paving the way for more precise tools to monitor chronic kidney disease (CKD). The next generation of wearable biosensors aims to replace invasive blood tests with continuous, non-invasive monitoring using sweat, saliva, and interstitial fluid (ISF). These devices will track critical biomarkers such as creatinine, urea, cystatin C, and potassium [1][5].
One promising technology is Organic Electrochemical Transistors (OECTs). These devices amplify signals to detect trace levels of biomarkers like cystatin C, even at nanomolar concentrations. This is particularly noteworthy because cystatin C offers a clearer picture of kidney function compared to creatinine, as it isn’t influenced by muscle mass [1]. Another exciting development involves Molecularly Imprinted Polymers (MIPs), which act as synthetic antibodies. Unlike traditional biological sensors, MIPs are more stable and easier to integrate into wearable devices [1].
In a notable example, Mode Sensors AS tested the Re:Balans® sensor in Norway between May and June 2021. This 15-gram adhesive patch monitored extracellular resistance every 30 seconds in 31 end-stage renal disease patients. The results showed a strong correlation (r = 0.82) between the sensor’s data and the actual fluid volume removed during dialysis [8].
Experts believe these innovations are nearing real-world application. John Rogers, PhD, Executive Director of the Querrey Simpson Institute for Bioelectronics at Northwestern University, highlighted this progress:
"The wearable sensors are just around the bend. The implantable devices will likely take some years due to the regulatory pathway" [12].
Similarly, Vishnuram Abhinav, a PhD student at the University of Bath, estimated a timeline of just a few years:
"Biosensors for kidney health are highly promising and are on a clear trajectory toward clinical integration... I believe it may take 3 to 5 years" [12].
These advancements set the stage for policy changes that could accelerate the adoption of these technologies, as outlined in the next section.
Regulatory Changes and Policy Updates in 2026
Two major initiatives launched in 2026 are streamlining the path for wearable technologies to reach CKD patients. Starting in January 2026, the FDA introduced the Technology-Enabled Meaningful Patient Outcomes (TEMPO) pilot. This program allows manufacturers to bypass some traditional premarket approval steps by submitting real-world performance data instead. The FDA uses this data to assess how effective these devices are in everyday use [14].
Later that year, on July 1, 2026, the Centers for Medicare & Medicaid Services (CMS) rolled out the Advancing Chronic Care with Effective, Scalable Solutions (ACCESS) model. This 10-year national program is designed to support Medicare beneficiaries with chronic conditions like CKD through digital health tools and better care coordination. The model moves away from fee-for-service payments, rewarding providers for improving outcomes like blood pressure control and diabetes management [13].
FDA Commissioner Marty Makary, M.D., M.P.H., emphasized the importance of these changes:
"This pilot supports innovative tools and a health care delivery model that could improve care for millions of Americans managing chronic disease" [14].
Michelle Tarver, M.D., Ph.D., Director of the FDA's Center for Devices and Radiological Health, echoed this sentiment:
"The TEMPO pilot will allow us to responsibly encourage innovation while collecting real-world evidence that may help us better understand how these devices perform for patients in their everyday lives" [14].
These regulatory efforts align with the FDA’s "Home as a Health Care Hub" initiative, which aims to shift chronic disease management from clinics to patients’ homes through wearable and remote monitoring technologies [14]. For CKD patients, this means easier access to tools that can continuously monitor their condition, helping to catch complications early and reduce the need for emergency interventions.
Conclusion
Wearable technologies are transforming the way chronic kidney disease (CKD) is monitored and managed. Rather than relying solely on invasive blood tests and occasional clinic visits that provide only brief glimpses into a patient’s health, these devices now offer continuous, real-time tracking of crucial biomarkers like creatinine, urea, and electrolytes [1][5]. This shift from periodic to ongoing monitoring allows for the early detection of complications that might otherwise go unnoticed - such as arrhythmias and hyperkalemia - before they escalate into more serious health issues [3][6]. For instance, studies have found arrhythmias in 34% of hemodialysis patients, with wearable single-lead ECG systems demonstrating an impressive 98.25% accuracy in identifying hyperkalemia [3][6].
Beyond clinical benefits, wearables empower patients by reducing the need for frequent clinic visits and enabling them to monitor their health from home. One participant in the VIEWER Trial highlighted this convenience:
"VIEWER made me more aware of my condition. We were able to check blood pressure right at home instead of going to doctor or ER, which was nice." - Study Participant 0036, VIEWER Trial [11].
This patient-first approach is further enhanced when wearable data is integrated with digital health platforms.
By combining continuous monitoring with digital health tools, healthcare providers can remotely track patients, identify concerning trends, and adjust treatments before issues worsen. This is especially critical given the 10-fold increase in emergency department visits observed in the 30 days leading up to dialysis initiation [11]. Early detection and intervention through these technologies can help prevent such crises, improving overall patient outcomes.
For the 10–15% of American adults living with CKD [1], these advancements are reshaping care. Wearable technologies are not just improving quality of life - they’re redefining how CKD is managed, paving the way for proactive, tech-driven healthcare solutions.
FAQs
How can wearables help detect complications from chronic kidney disease early?
Wearable devices are becoming essential tools in spotting complications related to chronic kidney disease (CKD) early. By continuously monitoring vital signs, fluid levels, and key biomarkers, these devices deliver real-time data that can highlight potential problems before symptoms even appear.
Thanks to their non-invasive and consistent tracking capabilities, wearables give both patients and healthcare providers valuable insights. These insights enable timely adjustments to treatment plans, helping to lower the risk of serious complications and enhance the overall management of the disease.
What biomarkers do wearables track to help manage chronic kidney disease (CKD)?
Wearable devices have the capability to monitor essential biomarkers that play a crucial role in managing chronic kidney disease (CKD). These include creatinine levels, electrolyte balances - such as potassium, which is vital for identifying hyperkalemia - fluid retention, and cardiovascular metrics like blood pressure and heart rhythm. Keeping track of these indicators can aid in the early detection of kidney problems and provide valuable insights for ongoing care.
When paired with AI-powered health apps, advanced wearable technology can transform this data into actionable insights. This empowers individuals to make informed decisions to better manage their kidney health and improve overall well-being.
How do wearable devices help monitor chronic kidney disease (CKD)?
Wearable devices have become essential tools for managing chronic kidney disease (CKD). They continuously gather crucial health metrics like heart rate, fluid levels, and other vital signs. Equipped with sensors, these devices monitor changes in real time and send the data wirelessly to digital health platforms for further analysis.
By leveraging advanced algorithms, these platforms can identify patterns or early warning signs of potential complications, such as fluid overload or abnormal heart rhythms. This allows healthcare providers to remotely track a patient’s progress, adjust care plans to fit individual needs, and step in early when intervention is required.
For example, platforms like Healify take this a step further by combining wearable data with lifestyle information. They provide actionable insights that help patients take charge of their CKD management, all while cutting down on the need for frequent in-person clinic visits.
Related Blog Posts
Wearables are changing how chronic kidney disease (CKD) is monitored and managed. These devices offer non-invasive, real-time tracking of key biomarkers like creatinine, urea, and potassium, enabling earlier detection of complications such as arrhythmias and hyperkalemia. For the 37 million Americans living with CKD, this technology reduces reliance on blood tests and clinic visits, providing a more convenient and continuous way to monitor health.
Key Takeaways:
CKD affects 15% of U.S. adults, with late diagnosis often leading to irreversible damage.
Traditional tests are expensive, time-consuming, and provide only a single snapshot of kidney health.
Wearables track biomarkers through sweat and interstitial fluid, offering continuous insights into kidney function.
Devices like the Lepu ER1 and Withings Scanwatch detect heart issues and other complications with high accuracy.
Integration with digital platforms allows remote monitoring, enabling healthcare providers to intervene earlier.
Wearables are reshaping CKD care by making monitoring more accessible, precise, and patient-friendly.

Traditional CKD Monitoring vs Wearable Technology: Key Differences and Benefits
Wearable Sensor for kidney disease
How Wearable Technologies Monitor CKD
Wearable devices are transforming kidney health monitoring by offering a non-invasive way to track key biomarkers in real time. Unlike traditional blood tests that require trips to the lab and waiting for results, these devices analyze biofluids like sweat and interstitial fluid (ISF) on the spot. This real-time monitoring makes it possible to detect changes in kidney function earlier and track biomarkers more precisely over time.
Key Biomarkers for CKD Monitoring
Wearables focus on critical biomarkers like creatinine, urea, and cystatin C to estimate eGFR, the standard measurement for kidney function. For example, creatinine - one of the most important indicators of kidney health - can be measured in ISF at levels of 45–110 μM, which closely match those found in blood. This makes ISF a practical alternative to traditional blood tests [1]. Urea levels, which increase as kidney function declines, are another key marker for managing chronic kidney disease.
Cystatin C is gaining attention as a reliable biomarker because its levels are not influenced by muscle mass. Its typical blood concentration ranges from 60–90 nM, but detecting it requires highly sensitive technology [1]. Wearables also monitor electrolytes like potassium, sodium, and calcium. For instance, potassium levels above 6.0 mmol/L signal severe hyperkalemia [3], offering insights into kidney health and overall fluid balance. These biomarkers are captured using advanced, non-invasive sensing techniques.
Non-Invasive Sensing Technologies
Modern wearable devices use cutting-edge, non-invasive methods to measure biomarkers. For instance, sweat analysis is a common approach that employs iontophoresis - a mild chemical stimulation (often with pilocarpine) - to induce sweat production even when the body is at rest [1][7]. The sweat is then analyzed using electrochemical sensors, which rely on enzymatic reactions like creatinine deiminase to break down creatinine for detection.
Another method is interstitial fluid sensing, where devices use microneedle patches or reverse iontophoresis (a small electrical current that extracts molecules) to access ISF [1][9]. This method is particularly effective for tracking larger molecules, such as cystatin C, which are less detectable in sweat.
Advances in sensor technology are improving the accuracy of these measurements. Molecularly Imprinted Polymers (MIPs), for example, act as synthetic receptors that are more stable than natural antibodies [1][9]. Similarly, Organic Electrochemical Transistors (OECTs) amplify weak signals, making it easier to detect even trace amounts of biomarkers. Some devices also incorporate colorimetric methods, where chemical reactions cause color changes that can be analyzed using smartphone cameras [1][7]. To ensure reliable results, advanced wearable patches include features like pH and sweat rate sensors to adjust readings and minimize interference.
Wearables for Tracking CKD-Related Health Metrics
Wearable devices are transforming how we monitor and manage chronic kidney disease (CKD). These gadgets continuously track vital signs that are critical for CKD care, especially since cardiovascular complications account for 48% of deaths among stage 5D CKD patients. For those dependent on dialysis, the mortality rate is a staggering 10 to 20 times higher than in the general population [4]. The constant stream of data from wearables supports precise interventions, improving both heart health and overall CKD management.
Monitoring Vital Signs and Related Conditions
Wearables are particularly effective in tracking the vital signs that help manage cardiovascular complications linked to CKD. For example, the BPM Connect provides automated blood pressure readings with a minimal margin of error - just 0.6 ± 5.3 mmHg for systolic measurements. Heart rate variability (HRV) is another critical metric. A study involving 458 patients, known as the CRIC study, demonstrated that HRV strongly predicts cardiovascular risk. It found that patients with high proteinuria had an SDNN (a key HRV metric) that was 5.73 ms lower. Those with an SDNN below 50 ms faced a 51.4% mortality risk, compared to just 5.5% for those with an SDNN above 100 ms [4][2].
Fluid management, another cornerstone of CKD care, also benefits from wearable technology. Bioimpedance sensors, like the Re:Balans used in a Norwegian study, track extracellular resistance (RE) changes during dialysis. Among 31 end-stage renal disease patients, RE increased by an average of 7.5 ± 4.3 Ω, correlating strongly (r = 0.82) with the volume of fluid removed [8]. Meanwhile, the Withings Scanwatch offers a 3% RMSE for SpO2 readings, aiding in early detection of issues like volume overload and pulmonary edema [4].
Advanced algorithms applied to wearable ECG data can even detect hyperkalemia with an accuracy of around 98% [3]. This is a game-changer, as serum potassium levels above 6.0 mmol/L are linked to significantly higher risks of complications and death. Noninvasive monitoring through wearables helps prevent such emergencies.
Stress and Sleep Tracking for CKD Patients
Wearables go beyond cardiovascular metrics, offering insights into stress and sleep - both of which are crucial for CKD care. Sleep disorders are a common issue, with 69% of maintenance hemodialysis patients experiencing insomnia, 24% dealing with obstructive sleep apnea, and 18% suffering from restless leg syndrome [4]. These issues are even more pronounced in stage 5 CKD patients and are associated with poorer quality of life and worse health outcomes.
The Withings Sleep Analyzer uses pressure sensors to track sleep stages, heart rate, and breathing patterns. It has shown 88% sensitivity and 88.6% specificity in detecting moderate-to-severe sleep apnea (AHI ≥ 15) [4].
HRV metrics also shed light on the autonomic nervous system. CKD patients with diabetes often show disrupted circadian rhythms [2][10]. Wearables can monitor nocturnal blood pressure and heart rate dipping, which, when absent, is linked to higher cardiovascular risks and mortality [2]. Additionally, advanced sensors like Organic Electrochemical Transistors (OECTs) can detect cortisol levels in sweat at nanomolar concentrations, offering insights into stress levels [1].
Platforms like Healify integrate data from wearables - covering HRV, sleep patterns, and stress markers - into actionable health plans. Healify’s AI health coach, Anna, provides personalized recommendations to help patients manage CKD and maintain cardiovascular health, creating a more holistic approach to care.
Connecting Wearable Data with Digital Health Platforms
When wearable devices sync with digital health platforms, they turn raw data into meaningful insights that can drive early medical intervention. For patients with chronic kidney disease (CKD), this integration allows healthcare providers to monitor key health trends remotely and step in before complications escalate.
Remote Monitoring and Clinical Decision Support
Wearables send data through Bluetooth, WiFi, or cellular networks to secure cloud platforms. Healthcare providers can then access this data using web dashboards that display trends, alerts, and clinical notes, offering a clear view of patient health [4][11]. This kind of connectivity is crucial - studies show that emergency visits spike tenfold in the 30 days leading up to dialysis [11].
A practical example of this approach is the VIEWER trial, conducted from November 2017 to July 2019 at Seven Oaks General Hospital in Winnipeg, Manitoba. Dr. Claudio Rigatto and his team equipped 26 advanced CKD patients (eGFR <15) with iPad minis and Bluetooth-enabled devices to monitor blood pressure, weight, and oxygen saturation. The system effectively tracked uremic symptoms and vital signs, but adherence dropped from 77.17% initially to 36% over three months. The decline was largely due to connectivity issues with Bluetooth devices and the perceived inconvenience of use [11].
The Withings RPM Solution provides another real-world application. Devices like the ScanWatch sync with a centralized cloud system where data is processed on HDS servers. Patients can view their metrics through the Health Mate app, while healthcare providers rely on a web-based interface for clinical decisions. Bernard Canaud from Fresenius Medical Care's Global Medical Office highlighted the benefits of this technology:
"technological advances had led to the development of new home-used, self-operated, connected medical devices, which offer convenient and new tools for monitoring patients in a fully automated and ambulatory mode" [4].
This seamless data integration creates a foundation for artificial intelligence (AI) systems to refine these insights and enhance patient care.
AI-Powered Analysis for CKD Management
Once wearable data is securely transmitted and aggregated, AI models step in to turn these metrics into actionable clinical insights. For instance, Convolutional Neural Networks (CNNs) can process raw sensor data - like ECG waveforms - to detect specific health issues without manual input [3]. Notably, 80.8% of arrhythmias identified by wearable ECG monitors in hemodialysis patients were asymptomatic, highlighting the importance of continuous AI-driven monitoring [6].
Between March 2022 and October 2023, researchers at the West China Biomedical Big Data Center of Sichuan University developed an advanced monitoring system for over 500 hemodialysis patients. Using a wearable chest strap ECG paired with a 1D-CNN model, the system achieved 98.25% accuracy and 98.63% sensitivity in identifying serum potassium levels above 6.0 mmol/L. This high level of precision enables timely interventions to prevent life-threatening hyperkalemia [3].
Healify takes this integration a step further by combining wearable data with personalized AI-driven insights. The app’s AI health coach, Anna, analyzes metrics like heart rate variability, sleep patterns, and stress levels alongside other biometrics and lifestyle factors. This comprehensive analysis provides 24/7 tailored recommendations, helping CKD patients manage their condition with clear, actionable plans that simplify complex health data.
The Future of Wearables in CKD Monitoring
New Developments in Wearable Biosensors
Advancements in wearable technology are paving the way for more precise tools to monitor chronic kidney disease (CKD). The next generation of wearable biosensors aims to replace invasive blood tests with continuous, non-invasive monitoring using sweat, saliva, and interstitial fluid (ISF). These devices will track critical biomarkers such as creatinine, urea, cystatin C, and potassium [1][5].
One promising technology is Organic Electrochemical Transistors (OECTs). These devices amplify signals to detect trace levels of biomarkers like cystatin C, even at nanomolar concentrations. This is particularly noteworthy because cystatin C offers a clearer picture of kidney function compared to creatinine, as it isn’t influenced by muscle mass [1]. Another exciting development involves Molecularly Imprinted Polymers (MIPs), which act as synthetic antibodies. Unlike traditional biological sensors, MIPs are more stable and easier to integrate into wearable devices [1].
In a notable example, Mode Sensors AS tested the Re:Balans® sensor in Norway between May and June 2021. This 15-gram adhesive patch monitored extracellular resistance every 30 seconds in 31 end-stage renal disease patients. The results showed a strong correlation (r = 0.82) between the sensor’s data and the actual fluid volume removed during dialysis [8].
Experts believe these innovations are nearing real-world application. John Rogers, PhD, Executive Director of the Querrey Simpson Institute for Bioelectronics at Northwestern University, highlighted this progress:
"The wearable sensors are just around the bend. The implantable devices will likely take some years due to the regulatory pathway" [12].
Similarly, Vishnuram Abhinav, a PhD student at the University of Bath, estimated a timeline of just a few years:
"Biosensors for kidney health are highly promising and are on a clear trajectory toward clinical integration... I believe it may take 3 to 5 years" [12].
These advancements set the stage for policy changes that could accelerate the adoption of these technologies, as outlined in the next section.
Regulatory Changes and Policy Updates in 2026
Two major initiatives launched in 2026 are streamlining the path for wearable technologies to reach CKD patients. Starting in January 2026, the FDA introduced the Technology-Enabled Meaningful Patient Outcomes (TEMPO) pilot. This program allows manufacturers to bypass some traditional premarket approval steps by submitting real-world performance data instead. The FDA uses this data to assess how effective these devices are in everyday use [14].
Later that year, on July 1, 2026, the Centers for Medicare & Medicaid Services (CMS) rolled out the Advancing Chronic Care with Effective, Scalable Solutions (ACCESS) model. This 10-year national program is designed to support Medicare beneficiaries with chronic conditions like CKD through digital health tools and better care coordination. The model moves away from fee-for-service payments, rewarding providers for improving outcomes like blood pressure control and diabetes management [13].
FDA Commissioner Marty Makary, M.D., M.P.H., emphasized the importance of these changes:
"This pilot supports innovative tools and a health care delivery model that could improve care for millions of Americans managing chronic disease" [14].
Michelle Tarver, M.D., Ph.D., Director of the FDA's Center for Devices and Radiological Health, echoed this sentiment:
"The TEMPO pilot will allow us to responsibly encourage innovation while collecting real-world evidence that may help us better understand how these devices perform for patients in their everyday lives" [14].
These regulatory efforts align with the FDA’s "Home as a Health Care Hub" initiative, which aims to shift chronic disease management from clinics to patients’ homes through wearable and remote monitoring technologies [14]. For CKD patients, this means easier access to tools that can continuously monitor their condition, helping to catch complications early and reduce the need for emergency interventions.
Conclusion
Wearable technologies are transforming the way chronic kidney disease (CKD) is monitored and managed. Rather than relying solely on invasive blood tests and occasional clinic visits that provide only brief glimpses into a patient’s health, these devices now offer continuous, real-time tracking of crucial biomarkers like creatinine, urea, and electrolytes [1][5]. This shift from periodic to ongoing monitoring allows for the early detection of complications that might otherwise go unnoticed - such as arrhythmias and hyperkalemia - before they escalate into more serious health issues [3][6]. For instance, studies have found arrhythmias in 34% of hemodialysis patients, with wearable single-lead ECG systems demonstrating an impressive 98.25% accuracy in identifying hyperkalemia [3][6].
Beyond clinical benefits, wearables empower patients by reducing the need for frequent clinic visits and enabling them to monitor their health from home. One participant in the VIEWER Trial highlighted this convenience:
"VIEWER made me more aware of my condition. We were able to check blood pressure right at home instead of going to doctor or ER, which was nice." - Study Participant 0036, VIEWER Trial [11].
This patient-first approach is further enhanced when wearable data is integrated with digital health platforms.
By combining continuous monitoring with digital health tools, healthcare providers can remotely track patients, identify concerning trends, and adjust treatments before issues worsen. This is especially critical given the 10-fold increase in emergency department visits observed in the 30 days leading up to dialysis initiation [11]. Early detection and intervention through these technologies can help prevent such crises, improving overall patient outcomes.
For the 10–15% of American adults living with CKD [1], these advancements are reshaping care. Wearable technologies are not just improving quality of life - they’re redefining how CKD is managed, paving the way for proactive, tech-driven healthcare solutions.
FAQs
How can wearables help detect complications from chronic kidney disease early?
Wearable devices are becoming essential tools in spotting complications related to chronic kidney disease (CKD) early. By continuously monitoring vital signs, fluid levels, and key biomarkers, these devices deliver real-time data that can highlight potential problems before symptoms even appear.
Thanks to their non-invasive and consistent tracking capabilities, wearables give both patients and healthcare providers valuable insights. These insights enable timely adjustments to treatment plans, helping to lower the risk of serious complications and enhance the overall management of the disease.
What biomarkers do wearables track to help manage chronic kidney disease (CKD)?
Wearable devices have the capability to monitor essential biomarkers that play a crucial role in managing chronic kidney disease (CKD). These include creatinine levels, electrolyte balances - such as potassium, which is vital for identifying hyperkalemia - fluid retention, and cardiovascular metrics like blood pressure and heart rhythm. Keeping track of these indicators can aid in the early detection of kidney problems and provide valuable insights for ongoing care.
When paired with AI-powered health apps, advanced wearable technology can transform this data into actionable insights. This empowers individuals to make informed decisions to better manage their kidney health and improve overall well-being.
How do wearable devices help monitor chronic kidney disease (CKD)?
Wearable devices have become essential tools for managing chronic kidney disease (CKD). They continuously gather crucial health metrics like heart rate, fluid levels, and other vital signs. Equipped with sensors, these devices monitor changes in real time and send the data wirelessly to digital health platforms for further analysis.
By leveraging advanced algorithms, these platforms can identify patterns or early warning signs of potential complications, such as fluid overload or abnormal heart rhythms. This allows healthcare providers to remotely track a patient’s progress, adjust care plans to fit individual needs, and step in early when intervention is required.
For example, platforms like Healify take this a step further by combining wearable data with lifestyle information. They provide actionable insights that help patients take charge of their CKD management, all while cutting down on the need for frequent in-person clinic visits.
Related Blog Posts
Finalmente toma el control de tu salud

Finalmente toma el control de tu salud

Finalmente toma el control de tu salud



