Wearables are transforming healthcare by providing continuous, real-time data that helps predict and manage health conditions. Devices like smartwatches and fitness trackers collect metrics such as heart rate, sleep patterns, and activity levels. This data feeds into machine learning models that detect early signs of issues like cardiac arrests, diabetes, or stress-related conditions. Key takeaways:
- Continuous Monitoring: Wearables track health metrics 24/7, offering insights beyond traditional checkups.
- Predictive Insights: Algorithms analyze patterns to forecast health risks, enabling early interventions.
- Chronic Disease Management: Tools like Continuous Glucose Monitors (CGMs) and heart rate trackers help manage diabetes and cardiovascular conditions.
- Real-Time Alerts: Immediate notifications empower users and healthcare providers to act quickly.
- Market Growth: The wearable tech market is projected to reach $173.7 billion by 2030.
Although challenges like data accuracy, privacy concerns, and integration into clinical workflows remain, wearables are reshaping healthcare by shifting the focus from treatment to prevention.
AI for Health with Wearables, Chenyang Lu, Washington University in St. Louis
sbb-itb-f5765c6
How Wearables Generate Predictive Health Insights
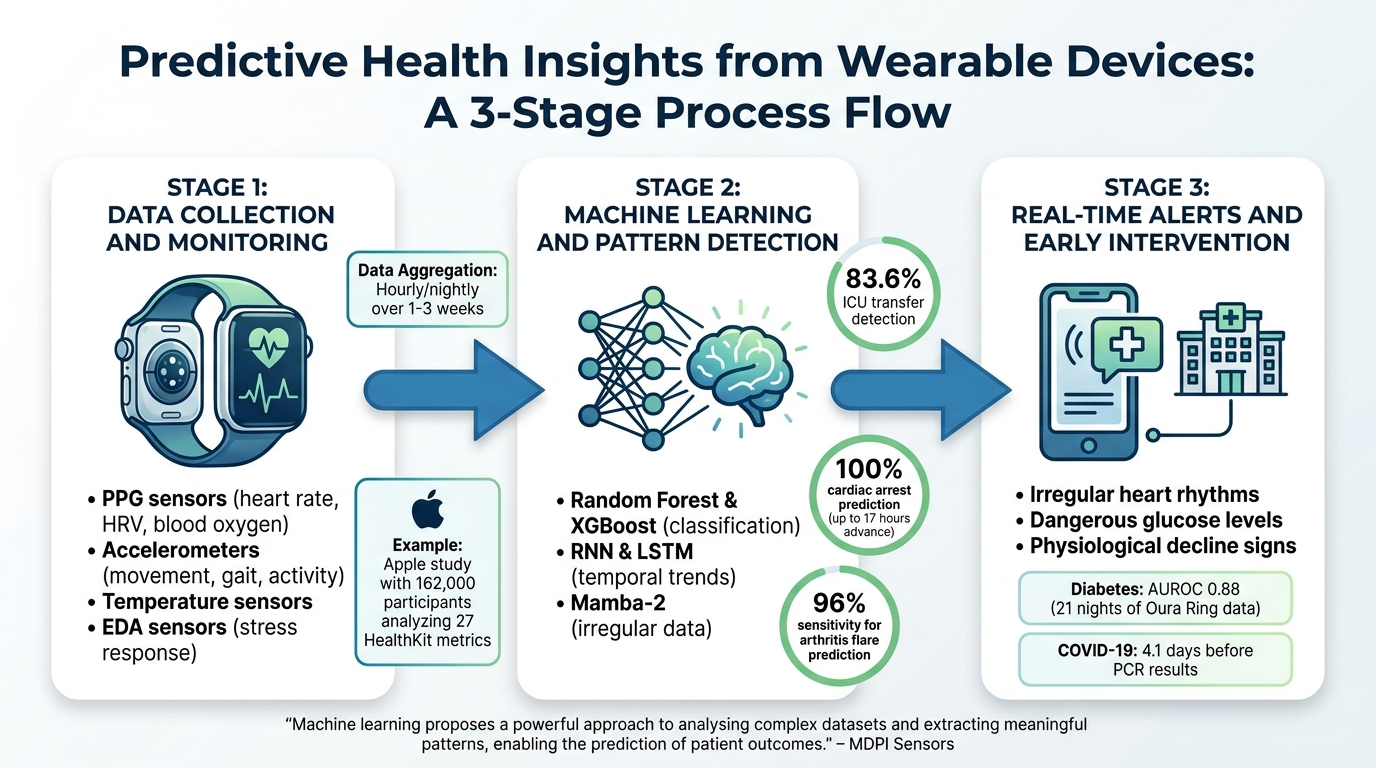
How Wearables Generate Predictive Health Insights: From Data Collection to Early Intervention
Wearable devices turn sensor data into actionable health predictions through a combination of data collection, advanced algorithms, and real-time alerts. This process helps identify potential health risks before they escalate into emergencies.
Data Collection and Monitoring
Modern wearables are equipped with a variety of sensors. For instance, photoplethysmography (PPG) sensors measure metrics like heart rate, heart rate variability, and blood oxygen levels. Accelerometers track movement, gait, and activity intensity. Some devices also include sensors for skin temperature and electrodermal activity (EDA) to monitor stress responses [1][3].
Organizing this data is just as important as collecting it. Wearables now focus on behavioral data - such as sleep patterns, walking steadiness, and mobility metrics - that reflect how conditions develop over time [5][8]. Data is typically aggregated hourly or nightly and analyzed over periods ranging from a week to three weeks to uncover chronic trends [5][11].
In July 2025, Apple researchers introduced a Wearable Health Behavior Foundation Model using data from 162,000 participants. This model analyzed 27 HealthKit metrics, including VO2Max and walking asymmetry, to predict 57 health-related tasks. By combining behavioral data with raw PPG readings, the model improved the detection of issues like hypertension and poor sleep quality [5][8].
Machine Learning and Pattern Detection
Machine learning algorithms are the backbone of wearable technology, revealing patterns in the complex datasets these devices generate. These algorithms can identify relationships - such as how physical activity impacts heart rate variability - which serves as a key indicator of resilience and recovery, that might not be apparent using traditional statistical methods [1].
Different types of algorithms are suited for different tasks. For example, Random Forest and XGBoost are often used for classification, while Recurrent Neural Networks (RNN) and Long Short-Term Memory (LSTM) models are better for capturing temporal trends in continuous data [4][10]. Advanced models like Mamba-2 can even process irregularly sampled data, accounting for times when the device isn’t worn [5].
"Machine learning proposes a powerful approach to analysing complex datasets and extracting meaningful patterns, enabling the prediction of patient outcomes." – MDPI Sensors [1]
Between March 2020 and November 2022, researchers applied an RNN model to data from 888 non-ICU patients across four hospitals. The model predicted unplanned ICU transfers and cardiac arrests with impressive accuracy - identifying 83.6% of transfers and all cardiac arrests up to 17 hours in advance [4]. Another study used a Naïve Bayes Classifier to analyze three months of step data, predicting rheumatoid arthritis symptom flares with 96% sensitivity [1].
These predictions trigger alerts that allow for timely interventions.
Real-Time Alerts and Early Intervention
Real-time alerts are a critical feature of wearable technology, enabling immediate action when concerning patterns are detected. For example, wearables can notify users of irregular heart rhythms, dangerous glucose levels, or early signs of physiological decline, giving healthcare providers a chance to intervene before conditions worsen [12][13].
A 2026 analysis of the TemPredict database highlighted how wearables can aid in chronic disease detection. Using data from 11,209 individuals, researchers analyzed 21 nights of sleep and distal body temperature data from the Oura Ring to detect diabetes with an AUROC of 0.88 [11]. For acute conditions, Oura Ring data proved highly effective, identifying COVID-19 infections an average of 4.1 days before PCR test results [9].
This combination of data collection, machine learning, and timely alerts directly supports better clinical decisions and proactive healthcare.
Using Wearables for Chronic Disease Management
Wearable technology has moved beyond early detection to play an active role in managing chronic diseases. By continuously collecting physiological data, these devices enable patients and healthcare providers to identify warning signs and adjust treatments in real time.
Diabetes Management
Continuous Glucose Monitors (CGMs) have revolutionized diabetes care by replacing traditional finger-prick tests with continuous glucose tracking. These devices monitor interstitial glucose levels throughout the day, giving users a clear picture of how factors like meals, exercise, and stress affect their blood sugar. Notably, CGMs were featured in 70% of studies focusing on AI and Type 2 Diabetes management [10][15].
In addition to glucose tracking, wearables now assess diabetes risk using non-invasive biomarkers. For example, an analysis of Oura Ring data in early 2026 involving 11,209 individuals over 21 nights revealed a 0.88 AUROC in identifying diabetes risk based on sleep and body temperature patterns. This is especially critical since approximately 8.5 million U.S. adults - 23% of the 37.1 million with diabetes - remain undiagnosed [11]. Metrics like heart rate variability and circadian temperature changes can signal metabolic issues even before blood sugar levels shift into abnormal ranges.
The WEAR-ME study, conducted through the Google Health Studies app with 1,165 participants, integrated data from Fitbit and Google Pixel Watch with routine blood biomarkers. This approach achieved a 0.88 AUROC in predicting insulin resistance and flagged 20% of participants with normal blood sugar as already insulin resistant. A Wearable Foundation Model, trained on 40 million hours of sensor data, helped identify these individuals before they progressed to diabetes [14].
"Identifying IR [insulin resistance] early can guide several focused lifestyle interventions, such as weight loss, regular exercise and a healthy dietary pattern, that can substantially improve or even reverse IR." - Nature [14]
Cardiovascular Health
Just as wearables help detect metabolic risks, they are also valuable for monitoring cardiovascular health. Metrics like resting heart rate (RHR) and heart rate variability (HRV) provide continuous insights into the autonomic nervous system and cardiovascular stress levels. Devices equipped with ECG capabilities can detect irregular heart rhythms, such as atrial fibrillation, which increases the risk of stroke and affects millions of Americans.
This continuous monitoring is vital as cardiovascular disease claimed 19.8 million lives globally in 2022, with about 34% of deaths occurring before the age of 70 [16]. Wearables can catch anomalies that might go unnoticed during routine checkups. Features like pulse wave velocity measurements help assess vascular stiffness, an early sign of arterial disease, while photoplethysmography (PPG) sensors track blood oxygen levels and circulation patterns. These tools refine predictive health models, making early intervention possible.
Sleep and Stress Management
Sleep tracking has advanced significantly, moving from basic duration measurements to detailed stage analysis. Modern wearables now differentiate between light, deep, and REM sleep, offering insights into overall health. Poor sleep quality is linked to insulin resistance, cardiovascular risks, and cognitive decline. By analyzing sleep stages, wearables can highlight patterns associated with metabolic issues.
Stress monitoring uses metrics like HRV and electrodermal activity (EDA) to assess the balance of the autonomic nervous system. Chronic stress, often reflected in these measurements, can have far-reaching health impacts. With only 17.4% of the estimated 96 million U.S. adults with prediabetes aware of their condition [11], tracking sleep and tracking stress levels offers an accessible way to detect metabolic risks early. Beyond daily well-being, these insights enhance predictive models for managing chronic diseases.
Case Studies: Wearables in Clinical Settings
These clinical studies showcase how wearable technology is making a difference in patient monitoring. They demonstrate the practical application of predictive health models using wearable devices in real-world clinical environments.
Apple Watch and Atrial Fibrillation Detection
The Apple Watch has shown its ability to detect irregular heart rhythms, specifically atrial fibrillation (AF), in clinical research. Using photoplethysmography (PPG) sensors, the device identifies new-onset AF - a condition linked to an increased risk of stroke. A study from January 2026 explored wearable-derived data to calculate "electrocardiographic age", a metric reflecting cardiovascular health in relation to a person’s chronological age. This measure acts as a biomarker for AF risk [17].
Unlike traditional in-hospital monitoring, continuous ambulatory monitoring with wearables captures real-life variations in heart rate and activity. For example, convolutional neural network models using wearable data achieved an F1 score of 0.56 and an area under the ROC curve (AUC) of 0.77, compared to 0.73 for conventional clinical measures. These models processed over 143 million heart rate data intervals, offering a more dynamic approach to patient monitoring [17].
"Wearables offer an exciting possibility for patient-directed data collection that better reflects real-life day-to-day variations in heart rate and physical activity."
– Nature Medicine [17]
Fitbit devices have also demonstrated their usefulness in predicting patient outcomes, particularly after hospital discharge.
Fitbit and Hospital Readmission Predictions
Hospital readmissions are a significant challenge, with roughly 20% of discharged patients returning within 30 days [19]. Fitbit data has shown potential in predicting these readmissions, allowing healthcare teams to take early action. Between January 2017 and December 2019, the University of Pennsylvania conducted the PREDICT trial, involving 500 patients discharged from medical services. Under the leadership of Dr. Mitesh S. Patel, the study revealed that integrating remote patient monitoring data improved the accuracy of predicting 30-day readmissions, raising the AUC from 0.72 to 0.85 [19].
Wearables provide dynamic insights into post-discharge activity and sleep patterns - data that static in-hospital monitoring cannot offer. For instance, wearables capture detailed sleep metrics, such as total, light, and deep sleep, which smartphones typically cannot. This additional information slightly improved predictive performance, with wearables achieving an AUC of 0.85 compared to 0.84 for smartphones [19].
In April 2025, researchers at the University of Pittsburgh Medical Center presented findings at Heart Rhythm 2025. Dr. John Kundrick and his team analyzed data from 14,000 participants in the NIH’s All of Us Research Program. Using machine learning to process Fitbit heart rate and step count data, they developed a model that predicted all-cause hospitalizations with 91% accuracy [18].
"We were surprised and encouraged by how robust the performance of some of the models were in regard to accuracy, area under the receiver operating characteristic curve, and F1 score."
– John Kundrick, MD, MPH, University of Pittsburgh Medical Center [18]
Integration with AI Platforms like Healify
AI platforms like Healify are reshaping the way wearable data is used, turning raw metrics into precise, actionable insights. By combining wearable tech with AI, these platforms create predictive health models that translate continuous data streams into meaningful health interventions.
Real-Time Health Monitoring in Healify
Healify gathers data from wearables - tracking metrics like heart rate, ECG, blood pressure, and sleep patterns - to build a personalized health profile for each user. Instead of relying on one-time readings, it uses ongoing data to establish a continuous health baseline. Machine learning algorithms then analyze this information to detect subtle changes in physiology, often before symptoms even surface. This allows the system to send immediate alerts for issues like irregular heart rhythms or low oxygen levels [12][13].
This kind of real-time monitoring is especially important considering that chronic diseases account for nearly 90% of the $4.1 trillion spent on healthcare annually in the U.S. [13]. By catching potential problems early through real-time alerts, Healify helps reduce the likelihood of costly emergency room visits or hospital stays. It’s not just about identifying problems - it’s about acting on them quickly, which is a game-changer for preventative care.
Personalized Health Coaching with Anna
Once continuous monitoring is in place, Healify takes it a step further with personalized health coaching. Anna, the platform's AI health coach, transforms wearable data into tailored recommendations. Using deep learning, Anna processes time-series data to spot patterns that might indicate upcoming health events [12][10]. Based on these insights, she provides specific advice on exercise, diet, and medication, all customized to how your body responds to different activities and foods.
This AI-driven coaching has a measurable impact, extending far beyond general wellness. For instance, 85% of surveyed physicians believe digital health tools are essential for personalized medicine, and 58% see AI as having the most significant influence on patient care [12]. Anna offers constant support, helping users manage chronic conditions, reduce stress, and improve sleep - areas where continuous data can reveal trends that standard check-ups might overlook.
Combining Wearable Data with Other Health Inputs
Healify’s true strength lies in its ability to integrate wearable data with other health inputs, such as bloodwork, genetic profiles, biometrics, and even lifestyle factors like diet and environmental exposures [13]. This combination of diverse data sources creates a more complete picture of an individual’s health. For example, the platform might link sleep patterns to blood glucose levels and stress markers to explain fluctuations in energy levels.
Studies show the potential of such integrations: 60% of reviews on AI-wearable systems report glucose prediction accuracy within clinically acceptable ranges (RMSE under 15 mg/dL) [10]. By synthesizing data from multiple sources, Healify doesn’t just track health - it crafts personalized strategies for prevention. This aligns with the belief of 93% of healthcare professionals who say personalized medicine can improve overall health outcomes [12].
Challenges in Using Wearables for Predictive Health
Data Accuracy and Reliability
Wearable sensors come with their own set of limitations, which can significantly impact the accuracy of predictive health models. For example, photoplethysmogram (PPG) sensors - those green LED lights commonly seen on wrist-worn devices - often struggle with precise measurements due to factors like skin tone, movement, or interference from sweat, lotion, or hair [20]. While these devices perform reasonably well when tracking resting heart rate (with a mean bias of about ±3–5 bpm), their accuracy takes a nosedive during high-intensity activities. During workouts, movement artifacts and unstable sensors can result in heart rate readings being off by as much as 12% [20].
The inaccuracies don’t stop there. When it comes to estimating energy expenditure, wearables show mean absolute errors ranging from 29% to a staggering 80%, making calorie-burn data far from reliable [20]. This lack of precision creates challenges for predictive health models that depend on accurate data inputs. As Cailin Madrigale, a Risk Management Analyst at ECRI, points out:
"Many nonprescription commercial wearable devices available to the public are not approved or regulated by the U.S. Food and Drug Administration (FDA), and all have varying degrees of accuracy, usability, privacy protections, and interoperability" [21].
Predictive models also face hurdles due to noise caused by sensor misplacement, motion artifacts, and external factors like caffeine or alcohol consumption. These issues are further compounded by the often imprecise or delayed nature of self-reported data [9]. Another concern is the lack of diversity in research - only 7% of studies on AI and wearables for diabetes management, for instance, reported racial and ethnic demographics [10]. This lack of representation can lead to "black-box" models that fail to serve underrepresented groups effectively. These sensor-related challenges highlight the complexities of integrating wearables into predictive health systems.
Clinical Integration and Scalability
Bringing wearable data into clinical settings is anything but straightforward. Between March 2020 and November 2022, researchers tested chest-worn wearable devices on 888 non-ICU inpatients across four hospitals. The system detected 126 more clinical alerts compared to manual monitoring and predicted adverse outcomes with 81.8% accuracy up to 17 hours in advance [4]. While these results are promising, they come with a downside: high-frequency monitoring can lead to alert fatigue. When clinicians are bombarded with notifications, they may dismiss important alerts, delaying critical interventions [4]. This underscores the need for platforms that can turn wearable data into actionable insights without overwhelming healthcare providers.
Continuous data streams also add to the workload of already overstretched clinicians. As Arjun Mahajan from Harvard Medical School explains:
"Provider adoption will depend not just on proving clinical value, but on developing streamlined workflows that allow physicians to efficiently incorporate continuous monitoring data into their practice without increasing their already heavy workload" [22].
Economic and policy barriers further complicate matters. The high cost of wearable hardware, the need for expensive digital infrastructure, and the absence of reimbursement models for the time clinicians spend analyzing wearable data all slow down adoption [10][22]. Another issue is that many AI models are trained on homogeneous datasets, raising concerns about their effectiveness across diverse populations [10][22]. Additionally, the "black box" nature of deep learning models makes it hard for clinicians to trust predictions when the underlying mechanisms remain unclear [1][10].
Privacy and Ethical Considerations
Beyond technical and workflow challenges, privacy and ethics are major concerns in the use of wearables for predictive health. The continuous collection and transmission of sensitive health data make these devices vulnerable to cyberattacks and data breaches [13][2]. Every time a wearable syncs with a cloud server, it creates a potential entry point for hackers. Furthermore, the use of non-diverse training data can lead to biased predictions, which may result in unequal health outcomes for underrepresented populations [13][10]. The opacity of complex deep learning models only adds to the problem. As highlighted in npj Digital Medicine:
"Complex 'black-box' models... pose barriers to clinical adoption due to limited transparency" [10].
If healthcare providers can’t fully understand or trust the predictions generated by these models, they’re unlikely to rely on them for clinical decision-making. This lack of trust could hinder the broader adoption of wearables in healthcare.
Conclusion: The Future of Wearables in Predictive Health
Wearables are transforming the way we approach chronic disease management, moving from periodic check-ins to a model of continuous, proactive care. While challenges remain, the integration of wearable data with Electronic Health Records (EHRs) has already shown promise, boosting prediction accuracy by an average of 8.5% across various clinical outcomes [7].
Looking ahead, predictive health models will rely more heavily on advanced tools like Wearable Foundation Models, which are trained on vast amounts of sensor data. These models can identify intricate physiological patterns that traditional methods might miss. For example, detecting insulin resistance early can lead to impactful lifestyle changes. As Nature highlights:
"Identifying IR [insulin resistance] early can guide several focused lifestyle interventions, such as weight loss, regular exercise and a healthy dietary pattern, that can substantially improve or even reverse IR" [6].
The real value of wearable data lies in its ability to be translated into actionable insights. Platforms like Healify are leading the way by combining wearable data with bloodwork, biometrics, and lifestyle information. Their AI health coach, Anna, simplifies complex data into practical recommendations - whether it’s adjusting sleep routines based on heart rate variability or tailoring dietary advice to glucose trends.
Emerging innovations, such as Liquid Neural Networks, will further revolutionize wearables by enabling them to adapt in real time to rapid physiological changes like blood sugar fluctuations [10]. These advancements pave the way for more precise interventions, improving outcomes for patients managing chronic conditions. The broader implications are reflected in the booming AI healthcare market, which is expected to surpass $187.95 billion by 2030, with a compound annual growth rate of 37% from 2022 [23]. Research by Will Ke Wang and colleagues underscores this potential:
"Wearable integration consistently improved model performance relative to EHR-only baselines, e.g., average delta AUROC +6.8% for major depressive disorder, +9.7% for hypertension, and +12.6% for diabetes" [7].
The future of predictive health lies not in simply collecting more data but in using that data wisely to improve lives and overall well-being. Wearables are at the forefront of this shift, offering a glimpse into a more informed, healthier future.
FAQs
How accurate are wearable health predictions?
Wearable health devices are getting better at predicting health outcomes, thanks to improved sensor technology and artificial intelligence. Research indicates that these devices can analyze data like heart rate, activity levels, and sleep patterns to estimate metrics such as sleep quality, risks of metabolic disorders, and even the early onset of diseases. While their accuracy varies based on factors like data quality, the condition being monitored, and the modeling methods used, wearables are proving to be valuable tools for proactive health management and early detection.
What wearable data is most useful for chronic disease risk?
Wearable devices collect key health metrics like blood pressure, heart rate, glucose levels, sleep patterns, body temperature, and physical activity. These data points play a crucial role in spotting early signs of chronic conditions such as cardiovascular problems, diabetes, and metabolic disorders. With real-time analysis, machine learning can highlight irregularities, predict potential risks, and guide tailored interventions, making it easier to manage chronic diseases proactively.
How does Healify turn wearable data into an action plan?
Healify leverages AI to transform data from wearables, biometrics, bloodwork, and lifestyle habits into tailored health recommendations. By offering real-time monitoring, it simplifies complex health metrics into actionable advice aimed at improving both physical and mental well-being. At the heart of this system is Anna, a 24/7 AI health coach. Anna provides ongoing support, offering strategies to reduce stress, improve sleep, and manage chronic conditions effectively, empowering users to take control of their overall wellness.
