Falls are a major health issue for older adults, affecting nearly 30% of those over 65 in the U.S. annually. These incidents lead to injuries, reduced independence, and over $50 billion in healthcare costs each year. Traditional methods often miss subtle risk factors, but AI is transforming fall prevention by predicting risks before they occur.
AI systems use data from wearable sensors, CT scans, and electronic health records (EHRs) to identify both immediate and long-term fall risks. For example:
- Wearable sensors monitor movement and gait patterns in real-time, detecting early signs of instability.
- AI-analyzed CT scans reveal frailty markers like low muscle density, offering insights traditional exams might miss.
- EHR-based models uncover systemic health issues, such as medication effects or chronic conditions, linked to falls.
These tools achieve high accuracy, with some models predicting falls with up to 99% precision within three months. By combining data sources, AI creates detailed risk profiles, enabling personalized interventions. Facilities using AI-driven systems have already reported significant reductions in falls.
AI isn’t just about prevention - it also empowers older adults with tools like health coaching apps, which provide tailored advice based on individual health data. This technology is making it easier to address fall risks proactively and improve quality of life for seniors.
Recent Studies on AI Fall Risk Prediction
Mayo Clinic Study Using Abdominal CT Scans
In early 2026, researchers at the Mayo Clinic introduced a novel way to assess fall risk by applying AI algorithms to abdominal CT scans. The AI analyzed core muscle density, uncovering frailty markers that traditional physical exams might overlook. This method, known as opportunistic screening, uses scans performed for other purposes to extract insights about fall risk. The study revealed a clear link: lower muscle density correlated with a higher likelihood of falls in elderly patients. This gives clinicians a more objective way to measure frailty. Meanwhile, sensor-based studies provide additional data by continuously monitoring movement patterns.
Wearable Technology with Surface Electromyography (sEMG) Systems
While imaging techniques focus on existing scans, wearable sensors provide real-time health adjustments. These devices, often equipped with 3-axis accelerometers, track movement continuously. Machine learning models process this data to predict falls with impressive accuracy[7]. By monitoring gait, physical activity, and physiological changes, these sensors can detect subtle shifts in behavior that might signal health declines[8]. AI also steps in to correct sensor inaccuracies, improving the reliability of predictions[9]. A team at Purdue University's Human Motor Behavior Group has developed AI tools to analyze motor behavior and gait patterns, with their findings published in PLoS ONE[6].
Machine Learning Models for Hospital Data Analysis
Machine learning models take a broader approach by analyzing hospital data to identify individuals at high risk of falls. These models process factors like age, medical history, and frailty markers to uncover patterns that might not be immediately obvious. A systematic review of 49 studies found performance values (AUC) ranging from 0.70 to 0.95. Interestingly, 87.8% of these studies relied on research-grade monitoring devices, while only 14.3% used commercial-grade wearables[8]. Unlike traditional methods, these models can sift through thousands of historical data points, identifying long-term risk factors such as medication effects and chronic conditions.
sbb-itb-f5765c6
How This AI Device Predicts Falls Before Seniors Fall | The PAUL System
Comparing Different AI Methods for Fall Risk Prediction
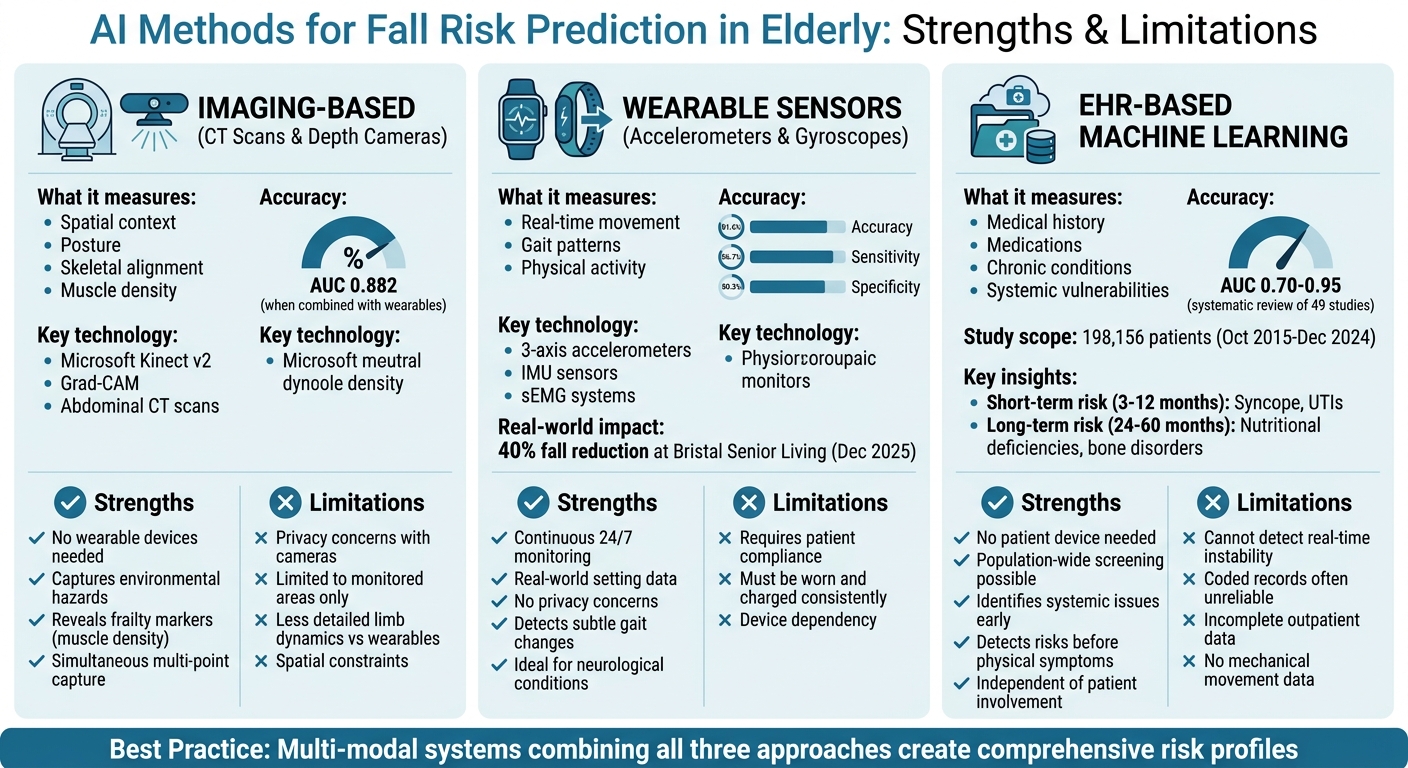
Comparison of AI Fall Risk Prediction Methods for Elderly Care
Strengths and Limitations of Imaging-Based Predictions
Imaging systems, like CT scans and depth cameras, are excellent for capturing spatial context. They can evaluate posture, skeletal alignment, and environmental hazards without requiring patients to wear any devices. Tools like Grad-CAM also enhance transparency by highlighting areas that are critical to assessing fall risks[10].
But imaging methods aren't without challenges. Privacy is a major concern, especially for camera-based systems, which often rely on silhouettes to protect identities[5]. These systems are also limited to specific monitored areas, making it hard to track a patient’s gait outside those zones. While imaging can simultaneously capture multiple key points, it generally falls short compared to wearable sensors when it comes to measuring detailed limb dynamics[13]. A study conducted at the City University of Hong Kong between December 2019 and January 2020 found that combining Microsoft Kinect v2 depth cameras with wearable sensors improved fall risk classification to an AUC of 0.882[13]. Because of these spatial limitations, researchers are increasingly turning to wearable sensors for real-time monitoring.
Benefits of Wearable Sensor Technology
Wearable sensors shine in real-world settings. Unlike lab-based assessments, which often reflect idealized conditions, these devices - equipped with accelerometers and gyroscopes - track how people move in their daily lives. They provide round-the-clock, objective data without raising privacy concerns[12]. For instance, a Random Forest model using wearable IMU data achieved 81.6% accuracy, 86.7% sensitivity, and 80.3% specificity in blind testing[11].
However, patient compliance is a significant hurdle. These devices only work when worn consistently and kept charged. Despite this challenge, they are particularly useful for individuals with neurological conditions like Parkinson’s or Alzheimer’s. Subtle gait changes, such as shorter steps or signs of muscle weakness, can indicate a heightened risk of falling[12]. A real-world example comes from the Bristal Senior Living facility in New York City, which, in December 2025, reported a 40% reduction in resident falls after adopting AI-driven sensor technology to monitor movement patterns and alert staff to concerning changes[5]. While wearables excel at tracking motion continuously, EHR-based models contribute insights from long-term medical histories.
How Machine Learning Performs in Data Analysis
EHR-based models complement sensor data by analyzing a patient’s comprehensive medical history. Instead of directly measuring movement, these models identify systemic vulnerabilities that might lead to falls, even before physical symptoms appear. Between October 2015 and December 2024, researchers at Froedtert Hospital in Milwaukee studied 198,156 patients using XGBoost and SHAP analysis. They discovered that short-term fall risks (3–12 months) were linked to acute conditions like syncope and urinary tract infections, while long-term risks (up to 60 months) were tied to chronic issues such as nutritional deficiencies[1].
"EHR-based prediction leverages the rich, longitudinal record of diagnoses, medications, and comorbidities to reveal underlying systemic vulnerability before overt physical decline." [1]
The major advantage of EHR-based models is their independence from patient involvement.
"Not all clinical settings are able to provide patients with high-tech devices and sensors, nor can we expect patients to purchase such devices for themselves." - Diagnostic and Prognostic Research [14]
These models enable population-wide screening across healthcare systems without relying on patients to adopt or manage technology. However, they come with their own challenges. Coded health records often lack reliability, and outpatient data is frequently incomplete. Additionally, EHR-based models cannot detect the real-time mechanical instability that wearable sensors excel at capturing[14][1]. By combining imaging for spatial insights, wearables for continuous tracking, and EHR analysis for systemic patterns, a more comprehensive risk profile can be developed.
What's Next for AI in Elderly Fall Prevention
Multi-Modal Systems for Complete Monitoring
The future of fall prevention lies in combining data from various sources to create a more comprehensive picture of risk. Fall risk isn't something fixed - it evolves over time based on numerous factors. Multi-modal systems aim to connect the dots between immediate physical risks, like instability detected by wearable sensors, and deeper systemic issues uncovered in electronic health records (EHRs) [1].
These systems go beyond labeling someone as "high-risk." Instead, they provide detailed, time-based risk profiles. For instance, AI can differentiate between urgent triggers, such as a urinary tract infection or a fainting episode, and ongoing issues like poor nutrition that require sustained attention [1].
A study conducted between June 2021 and July 2023 in German care facilities highlights how this approach works. Using the LINDERA mHealth app, researchers combined smartphone video analysis with a 58-question survey to generate a Fall Risk Score. They found that a score of 45% indicated a fall might occur within six months, while a score of 24% suggested a fall risk over 24 months [4]. This kind of temporal tracking shifts the focus from occasional assessments to continuous monitoring.
By integrating data from wearables, health records, and other sources, AI can refine risk predictions and pave the way for tailored interventions designed to meet individual needs.
AI's Role in Personalized Health Coaching
Explainable AI (XAI) is reshaping how health coaching tools share risk information with patients and caregivers. Technologies like SHAP and LIME make it possible to pinpoint the specific factors - such as a particular medication, changes in walking patterns, or a recent infection - that contribute to someone's risk level [10]. This clarity helps deliver more targeted and effective guidance.
A great example of this is Healify (https://healify.ai), an AI-powered health coaching platform. Its virtual coach, Anna, analyzes data from wearables, biometrics, and lifestyle habits to provide real-time, individualized advice. Whether it's addressing acute concerns like breathing problems or managing chronic issues like poor nutrition, Anna translates complex health data into simple, actionable steps. This makes fall prevention more accessible by eliminating the need for patients to decode medical jargon or sensor data themselves. The goal is to empower users with clear, practical guidance tailored to their unique health journey.
Conclusion and Key Takeaways
How AI Is Changing Elderly Care
AI is transforming how we approach fall prevention for older adults by creating adaptable risk profiles that change over time. Research shows that short-term risks (spanning 3–12 months) often stem from acute health issues like syncope or urinary tract infections, while long-term risks (24–60 months) are linked to chronic conditions such as nutritional deficiencies and bone disorders [1].
This understanding allows healthcare providers to design interventions tailored to specific timelines. For example, short-term prediction models achieve an Area Under the Curve (AUC) of about 0.75, while long-term models can accurately identify nearly 80% of individuals likely to experience falls [1]. Additionally, AI-based gait analysis has proven effective in predicting falls, with a Fall Risk Score of 45% indicating a high likelihood of a fall within six months [4].
One of the most exciting advancements is the rise of explainable AI. Tools like SHAP give clinicians clear insights into what factors - such as dizziness, changes in medication, or infections - are contributing to a person’s fall risk [1][3]. This level of transparency turns fall prevention into a precise science, enabling targeted and actionable strategies instead of relying on broad assumptions.
These advancements are setting the stage for practical AI-driven solutions that empower older adults to take charge of their health.
Take Action with AI Health Solutions
Falls are a serious concern, with nearly 30% of adults over 65 experiencing a fall each year [1]. Globally, falls result in approximately 646,000 deaths annually [2]. The good news? AI is making it easier to take proactive steps toward prevention.
Healify (https://healify.ai) is one such tool, bringing advanced AI technology straight to your iPhone. Its health coach, Anna, uses data from wearables, biometrics, and lifestyle habits to deliver real-time, personalized guidance. Whether managing acute issues or addressing chronic risks, Healify simplifies complex health data into actionable advice - making fall prevention more accessible and effective than ever.
FAQs
What data does AI need to predict fall risk?
AI processes data collected from wearable sensors like accelerometers, gyroscopes, and orientation trackers. By applying advanced models - such as deep learning - it can identify activity patterns and pinpoint time-based dependencies that may indicate fall risks.
How accurate are AI fall-risk predictions in real life?
AI models designed for predicting fall risks have shown impressive accuracy in practical applications. Some have achieved accuracy rates exceeding 98% when identifying falls and assessing risks among older adults. These results underscore how AI can play a key role in enhancing fall prevention and improving safety for seniors.
How can I use AI insights to prevent a fall at home?
AI is stepping in to help reduce the risk of falls at home by analyzing data from wearable devices. These devices track subtle movement patterns, allowing advanced AI systems to spot early signs of instability. With this information, AI can offer personalized recommendations, like specific exercises or lifestyle changes, aimed at improving balance and reducing the likelihood of falls.
What’s more, explainable AI goes a step further by identifying the exact factors that increase fall risks over time. This insight enables timely interventions, helping individuals make adjustments to their routines and stay safer in their daily lives.
